Dry Eye and Ocular Surface Treatment Options in NYC
Providing Diagnosis and Treatment in Manhattan and Astoria, NY
After the comprehensive dry eye examination, a personalized treatment plan is created by Dr. Pamel and his associates to address the causes of each individual’s dry eye. Some of the treatments listed below are in office treatments while others are home therapy as part of ongoing management.
Click the dry eye treatment categories below to learn more about available dry eye treatment options:
Medications
At-Home Treatments
In-Office Treatments
Medications for Dry Eye
Cyclosporine A 0.5% (Restasis)
Restasis eye drops are the only FDA approved medical treatment for dry eyes. This drop taken twice a day helps to decrease inflammation on the surface of the eye. This inflammation from dry eye disease can lead to chronic damage to the ocular surface. Restasis often takes up 4-6 months of twice daily use to be fully effective.
Corticosteroid Drops and Ointments
These medications are usually used either alone or used in conjunction with cyclosporine, reduce signs and symptoms of dry eye. The use of corticosteroids for Dry Eye is off label as it has not been approved by the FDA. However a number of studies have shown that they reduce inflammation in patients with dry eye and ocular surface disease.
Antibiotics Drops and Ointments
Antibiotic drops and ointments, are used in cases of blepharitis or meibomian gland dysfunction. These medications are used to kill the bacteria in the glands and on the lid margins, as these bacteria break down the lipid layer.
Oral Antibiotics
Again these medications work to kill bacteria in the glands and on the lid margins but by a different route. It is difficult for drops and ointments to fully penetrate these glands so it is sometimes necessary to use oral medication. This is often used if you have rosacea or ocular rosacea.
At-Home Dry Eye Treatment Options
Dietary Supplements
Omega-3 nutritional supplements have been proven to significantly improve eye health and relieve dry eye symptoms. The supplements recommended by the doctors at the Dry Eye and Ocular Disease Clinic utilize a well studied and therapeutically formulated omega-3 based nutritional supplement to help relieve symptoms. Click here to receive more information on PRN brand of Omega -3 nutritional supplements.
Artificial Tears and Ointments
In the early stages of dry eye disease, the use of artificial tears is appropriate to supplement the tear film and provide more immediate relief. The effect of these drops is usually short lived. Lubricating ointments may provide relief during nighttime hours but they do not treat the source of the dryness. It is important to use the correctly prescribed topical artificial teardrops as the wrong ones can actually aggravate the condition due to the detergent-like preservatives they contain.
Warm Compress and Eyelid Scrubs
Warm compresses and eyelid scrubs help by providing a thicker, more stable lipid layer. The medicated eyelid scrubs prescribed by Dr. Pamel and his associates at the Dry Eye and Ocular Disease Treatment Center have been specifically chosen for their effectiveness. This is especially helpful in patients with meibomian gland dysfunction, rosacea, or blepharitis. A study on warm compresses was performed to evaluate efficiency and efficacy of various warm compresses. The warm compress used by the Dry Eye and Ocular Surface Disease Center has been evaluated as the most effective.
Humidifiers, Air filters, and Environmental Modifications
In some cases it is necessary to modify the environment you encounter on a daily basis. Both furnaces in the winter and air conditioning in the summer decrease the humidity in the air and excessive air movement dries out your eyes. Humidifiers put more moisture in the air. With more moisture in the air, your tears evaporate more slowly, keeping your eyes more comfortable. Many times large amounts of dust or other particulate matter in the air may worsen the symptoms of dry eye and use of a simple air filter will improve comfort.
Dry Eye In-Office Treatments
Mibo ThermoFlo
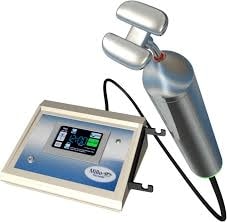
Meibography to assess the Miboflow Treatment Device
Evaporative dry eye is the leading cause of dry eye. Improving meibomian gland function is the mainstay of modern therapy. MiBo Thermoflo is a new treatment modality designed to address obstructed meibomian glands and foster superior lipid health and function. MiBo Flo is comfortable, effective, convenient, and affordable.
Dr. Pamel’s staff use a specially designed warming device is rested on the outside of the upper and lower eyelids.
This device delivers consistent heat to the meibomian glandular apparatus. Lipid secretions that have built up within the gland are softened and mobilized through gentle ocular message.
Improved lipid secretions can enhance the tear film leading to less evaporation and improved wetting of the cornea. Improved corneal wetting reduces or eliminates the signs and symptoms of ocular surface disease. This treatment can last between 3-4 months before it needs repeating.
Meibomian Gland Expression by Compression Forceps
Meibomian gland expression by compression forceps is utilized to help aid in clearing the meibomian glands from impaction and inspissation. Once the meibomian glands have been fully cleared of old lipid and cellular build up the glands have a chance to function at their full capacity.
BlephEx Treatment
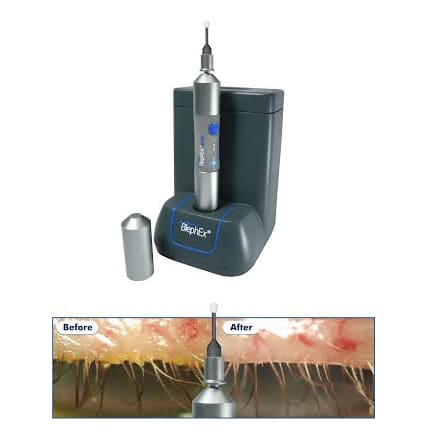
Blephex device for blepharitis treatment
Anterior blepharitis patients have loss of eyelashes, debris build up on the base of the lashes (collarettes) and redness on the eyelids and around the lashes. BlephEx is a painless in-office treatment performed by Dr. Pamel’s staff. A specially designed hand piece is used to very precisely and carefully, spin a soft medical grade micro-sponge along the edge of the eyelids and lashes, removing scurf and debris and exfoliating the eyelids. This sponge is disposable and a fresh clean one is used for each individual eyelid. The eyes are rinsed well afterwards.
The treatment takes about 6 -8 minutes and is well tolerated. Most patients simply report a tickling sensation. A numbing drop is usually placed in each eye prior to treatment for increased comfort.
After the treatment, the patient is instructed on how to maintain their clean eyelids with regular nightly lid hygiene. Since home treatments are only semi-effective, this treatment is typically repeated at 4-6 month intervals.
Amniotic Membrane Therapy
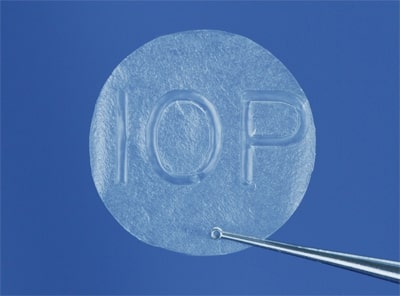
AmbioDisK: processed, dehydrated, sterilized human amniotic membrane tissue graft.
Amniotic membrane is an avascular fetal membrane that is harvested from the placenta at the time of elective Cesarean section. It is thin and semi transparent tissue. The amniotic membrane tissue has natural therapeutic actions that help damaged eye surfaces heal. Eyes treated with amniotic membrane tissue have quicker healing, less pain, less scarring, and less inflammation. It is a safe, effective treatment provided by a tissue bank regulated by the FDA.
In severe cases of dry eye and ocular surface disease, the use of amniotic membranes tissue can be utilized to promote healing of the damaged ocular surface. The tissue has passed many quality control tests before it is provided to Dr. Pamel and his associates at the Dry Eye and Ocular Surface Disease Center.
Punctal Occlusion
Near the inner corner of each eyelid are small openings, called punctae, responsible for tear drainage. Dr. Pamel and his associates perform a procedure known as punctal occlusion that can help dryness by decreasing the normal drainage of tears to help build and maintain a large tear reservoir.
This is a very simple office procedure and only takes a few minutes. Small plugs made of various materials are placed inside these openings to block drainage of tears. Just like a stopper that is put in the drain of a sink to keep the water from flowing down the drain, these plugs keep the tears that are made from flowing down the tear drainage system. Therefore, eyes stay moist and comfortable, even in those patients who produce fewer tears. These plugs are semi-permanent meaning they can easily be removed if necessary.
Dr. Pamel and his associates will first place the plugs in the lower lid openings and often that provides sufficient improvement in symptoms. In more severe cases, the upper punctae are plugged. In very severe cases of DES, these openings can be permanently closed, usually by cauterizing (burning) the opening to create a scar. This achieves the same objective as the plugs.
Therapeutic Prosthetic Scleral Devices and Scleral Lens Therapy
For individuals with vision affected by severe ocular surface disease, therapeutic prosthetics scleral devices and scleral lens therapy can help improve their quality of life by restoring vision and ocular comfort, as well as preventing further damage to the ocular surface. These devices are indicated for individuals with the most severe forms of dry eye and ocular surface disease.
Dr. Pamel and his team work extensively with therapeutic and visually rehabilitative devices and have helped suffering patients from all over the world. By utilizing the most advanced technology and fitting techniques combined with the latest materials and advanced designs, our doctors will determine the device for each individual.
These devices are specially designed to rest on the conjunctiva and underlying sclera, the “white” of the eye, and vault over the entire corneal surface. The cornea is one of the most sensitive tissues in the body and the one most damaged by dry eye and ocular surface disease. By vaulting over the cornea and resting on the much less sensitive sclera these devices can provide a relief and protection unseen in traditional treatments. The vaulting creates a space between the cornea and the back surface of the device. This space is filled with fluid and acts as a “tear bandage” which bathes the corneal surface to provide comfort, protection, and healing for people with diseases that affect the ocular surface.
This therapeutic use can rehabilitate the cornea and prevent further damage caused by various diseases. Examples include:
- Exposure keratitis
- Graft-versus-host disease
- Stevens Johnson Syndrome
- Severe dry eye caused by Sjögren’s syndrome, rheumatoid arthritis, or other inflammatory conditions
- Persistent corneal ulcers
Autologous Serum
Autologous serum is an artificial tear derived from you our blood. Autologous means that the donor and the recipient are the same person. Red blood cells and clotting factors are removed, leaving behind blood serum. The serum collected is diluted with a sterile preservative-free saline to produce a tear substitute that is unique to the patient. This autologous serum is rich in nutrients that are essential for comfort and healing in patients with dry eye and ocular surface disease.
Conjunctivoplasty
The conjunctiva is a clear saran wrap like tissue, it is the outermost layer on the “white” of the eye. When this tissue become loose or redundant (conjunctivochalasis) it can cause dry eye like symptoms including persistent foreign body sensation. Conjunctivoplasty or conjunctival resection surgery is a procedure used to eliminate redundant or loose conjunctival tissue from the front surface of the eye. These individual may in fact have accompanying dry eye however often the foreign body symptoms can be eliminated with this procedure.
Lateral Tarsorrhaphy
Lateral tarsorrhaphy is a procedure during which the lateral (outside) one-third of the eyelids are sewn together to decrease the exposed ocular surface area and reduce evaporation of the tear film. Dr. Pamel uses this technique in cases in which the eye cannot close properly from stroke or nerve damage causing the corneal surface to dry out (exposure keratitis).
Schedule Your Consultation for Dry Eye Treatment
To learn more about dry eye treatment in New York City, contact Pamel Vision and Laser Group by calling (212) 355-2215 or by visiting our website. Dr. Pamel will walk you through your diagnosis and treatment options, both in-office and at home.





